Early detection includes doing monthly breast self-exams, and scheduling regular clinical breast exams and mammograms.

Symptomes and signs

Breast pain

Learn about
breast cancer
most common cancer in women.
women will develop breast cancer in their life.



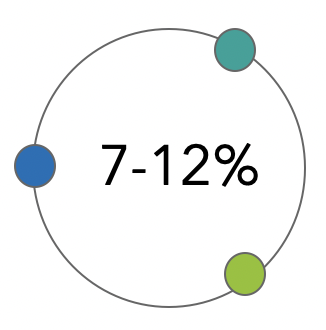
Source : Breast Cancer Surveillance Consortium
Source : ehrn.org
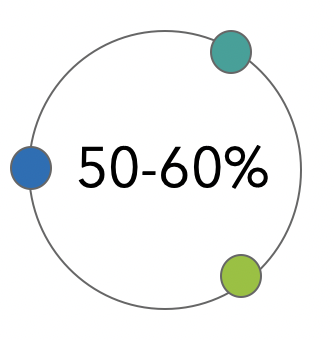
Decline in weekly screenings in March 2020.
Difference in screening imaging in US compared to June 2019 baseline.
285,000 estimated screenings missed or postponed between March and June 2020.





The American Cancer Society recommends that women aged 45–54 get mammograms every year, and women 55 and older can switch to a mammogram every other year or continue annual screenings. Women at high risk (due to family history or genetic factors) may need to start screening earlier. Talk to your doctor about what's right for you.
Some women experience brief discomfort during a mammogram because the breast is compressed between two plates. The compression is necessary to get a clear image, but it lasts only a few seconds per image. Most women describe the sensation as uncomfortable rather than painful. Scheduling your mammogram the week after your period, when breasts are less tender, can help reduce discomfort.
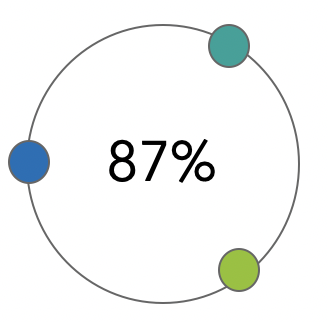
Our AI system analyzes mammogram images in under 2 seconds to flag suspicious areas for radiologist review. Studies show that AI-assisted reading increases radiologist sensitivity from an average of 87% to approximately 89%, while also helping to reduce false-positive rates. The AI acts as a first reader, helping experienced radiologists focus their attention on the areas most likely to need further evaluation.
If our AI and radiologist identify potentially concerning findings in your mammogram, our care team will contact you directly using the information you provided. We will guide you through the next steps, which may include additional imaging (such as an ultrasound or MRI) or a biopsy at one of our partner hospitals. Finding something suspicious does not necessarily mean cancer — many findings turn out to be benign upon further evaluation.